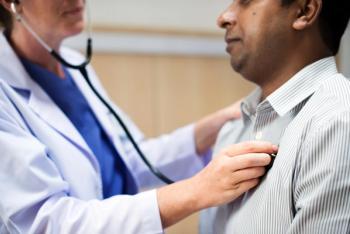
Providers must engage patients outside of appointments, Linnert said in an interview with Chief Healthcare Executive. Health systems can use their data to connect with patients.

Providers must engage patients outside of appointments, Linnert said in an interview with Chief Healthcare Executive. Health systems can use their data to connect with patients.

Many have avoided or delayed medical care during the COVID-19 pandemic. Employers should encourage their employees to get back into the habit of seeing doctors.

In an interview with Chief Healthcare Executive, Amwell’s senior medical director talks about the opportunities of telemedicine and some of the hurdles for the industry.

Consumers will be able to see which hospitals have the best outcomes. The Biden administration says it’s part of an effort to reduce maternal mortality.

The Leapfrog Group found a significant gap between the two in some areas. But Leah Binder, the group’s CEO, says both have room for improvement.

Doctors and executives see the value in the practice, but some say there are issues with workflows and reimbursement, a new survey finds.

The vast majority of doctors are using telehealth and see the value for patients. Some express concern about ensuring all patients can take advantage of it.

The Cleveland Clinic and Amwell have teamed up to offer patients, employers and health plans the chance to check a diagnosis remotely. Frank McGillin, CEO, says there’s a clear need and a substantial market.

Most executives describe it as a top priority, but only about a third have money allocated for health equity efforts. Ankoor Shah of Accenture outlines steps hospitals should consider.

The conference highlighted exciting opportunities for technology to dramatically improve healthcare, along with some formidable obstacles. Here are nine key takeaways from a memorable week.

More than 400 hospitals were honored with the Healthgrades 2022 Patient Safety Excellence Awards. The group’s report also cited four common incidents affecting the health of patients.

In an overview of the state of healthcare, leading experts talked about what needs to happen from the perspectives of providers, doctors, patients and payers.

Elsevier Health partnered with Ipsos for its first ‘Clinician of the Future’ report. Healthcare professionals say they’re worried about increasing technology demands and a shortage of doctors and nurses.
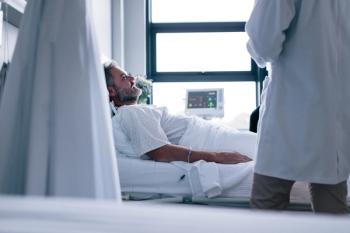
ECRI, a nonprofit group focused on improving safety in healthcare, has released its annual analysis. The group’s president offers suggestions for hospital leaders to protect patients.

A University of Michigan study looked at the factors adults 50-80 consider when deciding on surgery.

A study of online reviews revealed overt acts of racism, intimidation and dehumanizing treatment. Healthcare organizations should pay attention to those reviews and look for ways to get better.

The group examined hospitals with the highest volume of coronavirus patients in the first several months of 2020. Healthgrades’ chief medical officer says it’s a way to recognize providers who delivered exceptional care.

A recent study found evidence of bias in electronic health records. Michael Sun, the study’s lead author, talks about the implications and steps healthcare leaders should be taking.

More people are using telehealth and say they will continue to do so beyond the COVID-19 pandemic, according to Doximity. But there are differences in some groups worth noting.

The pandemic has wiped out years of progress in improving the safety of patients, federal officials say. More must be done to protect patients and workers, and more federal oversight could be in the mix.

Most healthcare executives say they’re worried inaccurate patient data is hurting outcomes and costing them money. The CEO of Verato says it’s something leaders must address.

The New York technology company’s software allows people to fill out paperwork and pay before appointments. Yosi Health offers convenience for providers and patients, CEO Hari Prasad says.

Only 12% of American adults are proficient in health literacy. Providers need to find ways to communicate with patients in ways they can understand.
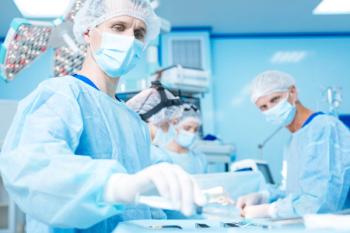
It's not a popularity contest. The focus is on patient outcomes, and top honorees must show consistency over time, the company says.

The Healthcare Executive Group surveyed its members as the industry deals with change at many levels.